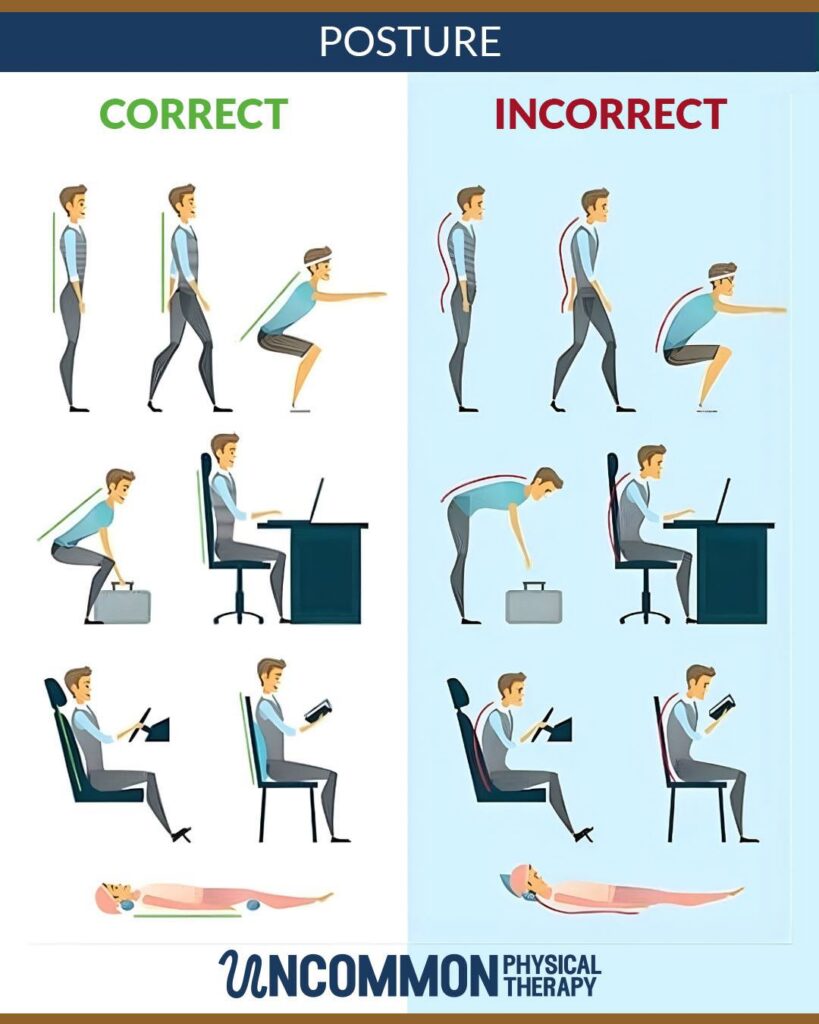
There’s a common pattern we see all the time:
You start moving more — maybe working out again, walking more, playing sports, or just trying to “be healthier” — and suddenly your body starts talking back.
A tight hamstring. A sore shoulder. A knee that feels… questionable. So you stretch more. Maybe rest a little. Maybe Google a few things. But the discomfort keeps coming back.
Here’s the truth that’s changing how people approach their health:
👉 It’s not just about moving more.
👉 It’s about moving better — and stronger.
At Uncommon Physical Therapy, we see this shift every day — and it’s one of the most important changes you can make for long-term health.
The Real Trend in Health: Strength Is the Foundation
For years, the focus was on stretching, foam rolling, and “loosening things up.”
Now, the conversation has evolved.
Strength training is one of the most powerful tools for:
- Reducing pain
- Improving mobility
- Protecting joints
- Enhancing balance
- Supporting long-term independence
And the best part? It works for every age group.
Common Misconception: “I Just Need to Stretch More”
Let’s clear this up: Feeling tight doesn’t always mean you need more flexibility.
In many cases, that “tight” feeling is actually:
- Weakness
- Lack of control
- Your body protecting an unstable area
So when you only stretch, you may get temporary relief — but not a lasting solution.
Quick Insight: Tight vs. Weak — What’s Really Going On?
If stretching “works”… but only for a few hours or days, you might be dealing with:
✔ Muscles that lack strength
✔ Joints that need more stability
✔ Movement patterns that need correction
What actually helps long-term:
➡ Strengthening the right muscles
➡ Improving control through movement
➡ Addressing the root cause (not just the feeling)
Why This Matters at Every Age
Teens & Young Adults
High activity + repetition = higher injury risk. Strength builds resilience and keeps you in the game.
Adults (30s–50s)
This is when small imbalances become chronic issues. Strength helps you stay active without setbacks.
60+
Strength directly impacts:
- Balance
- Fall prevention
- Independence
Translation: strength = longevity.
3 Simple Strength Habits That Make a Big Difference
You don’t need to overhaul your life — just start with intention.
1. Train Movements, Not Just Muscles
Focus on real-life patterns:
- Squatting
- Hinging
- Pushing
- Pulling
- Carrying
2. Slow It Down
Control builds stability. Rushing builds compensation.
3. Listen to Pain (Don’t Ignore It)
Pain is feedback — not weakness. It’s your body asking for a better strategy.
What Makes Strength Training Different at Uncommon PT
This is where things become… uncommon.
At Uncommon Physical Therapy, strength isn’t random — it’s personalized.
You’ll receive:
✔ One-on-one care every visit
✔ Hands-on treatment
✔ Targeted strength programming
✔ Movement analysis tailored to you
Because getting stronger only matters if it helps you move better and feel better in your daily life.
A Word From Our Team
“People think they need to slow down as they age — but what they really need is to build capacity. Strength gives your body options, and options are what keep you active, pain-free, and confident.”
– Davis Bradley, Owner
The Takeaway
More movement is good. But prepared movement is better. When your body is strong and supported, you don’t just move more —
you move with confidence, control, and freedom.
Ready to Build Strength That Actually Lasts?
If you’re dealing with:
- Recurring pain
- Stiffness that won’t go away
- Hesitation with movement
- You just want to feel stronger
We’re here to help.
📍 Uncommon Physical Therapy
6842 Carnegie Blvd, Suite 205
Charlotte, NC 28211
📞 (704) 803-8038
📧 Info@UncommonPhysicalTherapy.com
💬 Ask about our complimentary 15-minute phone consultation to see if we’re the right fit for you.
Stronger body. Better movement. Uncommon results.