Introduction
Dry needling has emerged as a prominent technique within physical therapy, offering a targeted approach for alleviating musculoskeletal pain and dysfunction. This section explores the historical development and foundational principles of dry needling, tracing its origins, evolution, and integration into modern physical therapy practice.
Historical Background
Dry needling, although often compared to acupuncture, has distinct roots and evolution. The practice of inserting needles into the body for therapeutic purposes dates back thousands of years in traditional Chinese medicine (TCM) with acupuncture. However, dry needling as it is practiced today in the West diverges significantly from TCM, focusing on the musculoskeletal system and utilizing a Western medical approach.
The term “dry needling” was first coined by Dr. Janet Travell in the 1940s. Dr. Travell, a pioneering American physician, is credited with developing the concept of myofascial trigger points and their role in pain syndromes. Her work, alongside Dr. David Simons, led to the publication of “Myofascial Pain and Dysfunction: The Trigger Point Manual” in 1983, which laid the groundwork for understanding and treating trigger points using dry needling techniques.
Foundations of Dry Needling
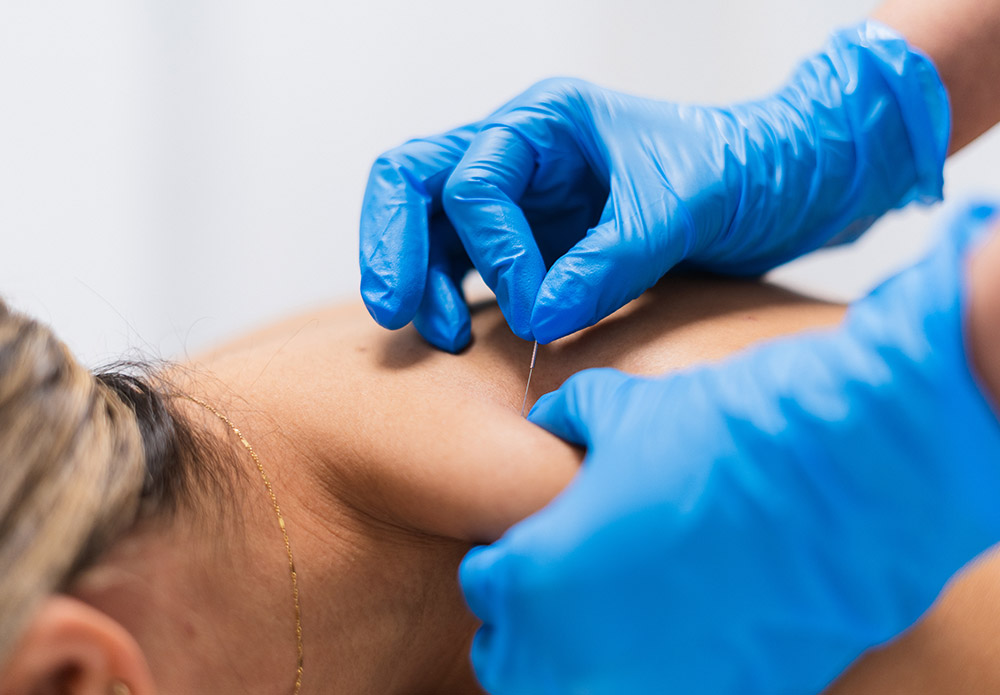
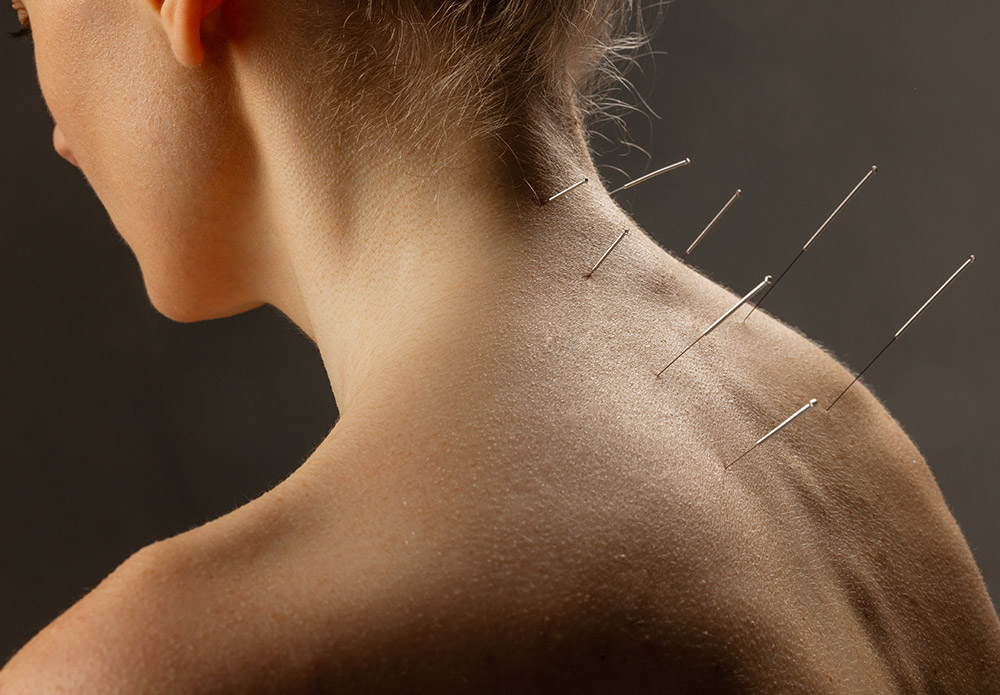
The core principle of dry needling lies in its focus on myofascial trigger points—hyperirritable spots within a taut band of skeletal muscle or fascia that are painful on compression. These trigger points can cause local pain and referred pain patterns, contributing to various musculoskeletal pain conditions.
Integration into Physical Therapy
The incorporation of dry needling into physical therapy practice has been driven by its efficacy in addressing musculoskeletal pain and dysfunction. Physical therapists, with their extensive training in anatomy, physiology, and musculoskeletal assessment, are uniquely positioned to utilize dry needling effectively and safely.
Clinical Applications
Dry needling is employed to treat a wide range of conditions. It is often used in conjunction with other therapeutic interventions, such as manual therapy, exercise, and modalities, to enhance overall treatment outcomes.
Evidence-Based Practice
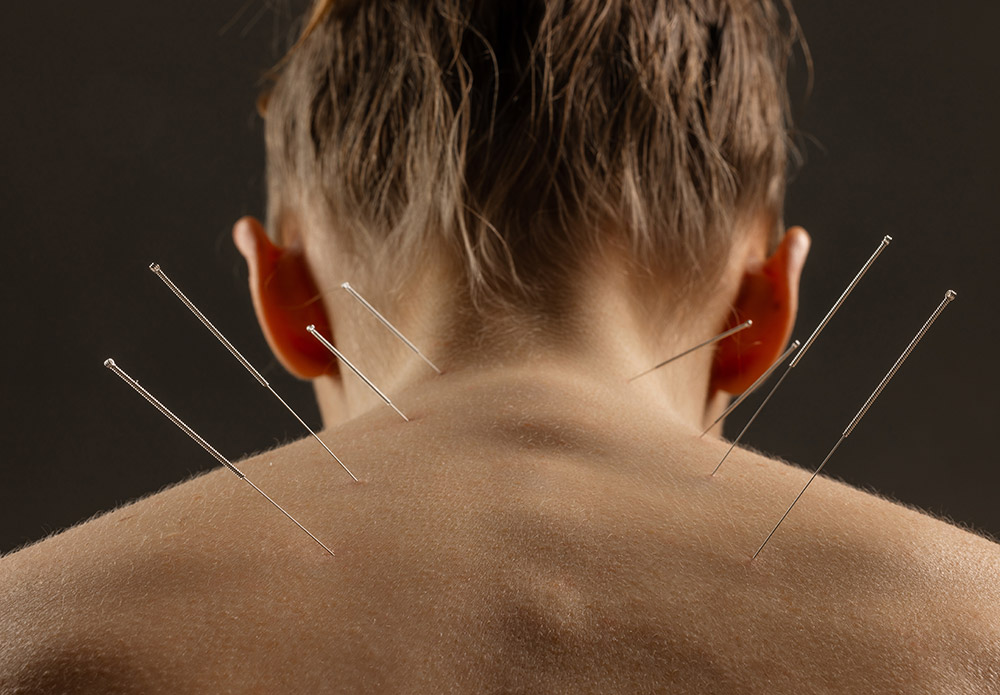
Numerous studies have demonstrated the effectiveness of dry needling in reducing pain and improving function in patients with musculoskeletal conditions. For example, a systematic review and meta-analysis by Kietrys et al. (2013) found that dry needling provided significant pain relief and functional improvements in patients with myofascial pain syndrome compared to sham or no treatment. Similarly, a randomized controlled trial by Mejuto-Borges et al. (2011) reported that dry needling of the trapezius muscle reduced pain intensity and improved cervical range of motion in patients with chronic neck pain.
Safety and Training
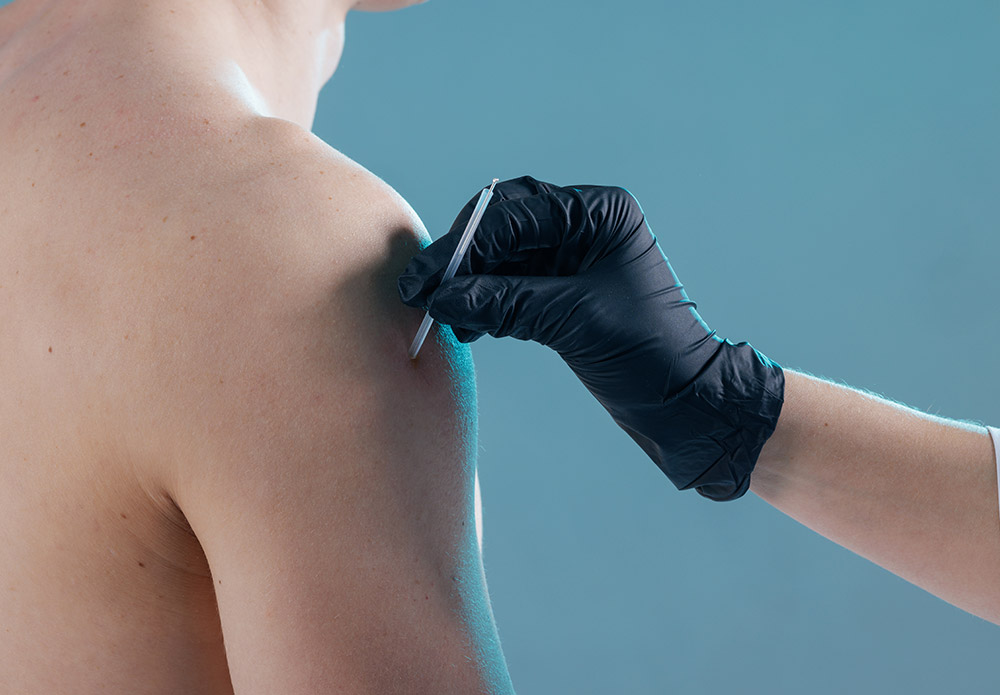
While dry needling is generally considered safe when performed by trained professionals, it is not without risks. Potential adverse effects include mild bruising, bleeding, soreness, and, in rare cases, more serious complications such as pneumothorax. Therefore, adequate training and adherence to safety protocols are essential. In the United States, the practice of dry needling by physical therapists is regulated at the state level, with varying requirements for training and certification. Many states require physical therapists to complete additional coursework and clinical practice hours to obtain certification in dry needling.
Conclusion
Dry needling has evolved from its historical roots into a well-established technique within physical therapy, offering a targeted approach to treating myofascial pain and dysfunction. Its foundations in trigger point theory, combined with evidence-based practice and integration into comprehensive treatment plans, make it a valuable tool for physical therapists. As research continues to expand our understanding of its mechanisms and applications, dry needling is likely to remain an integral component of modern physical therapy.
Free Consultation
Take advantage of a complimentary 15-minute phone conversation with a licensed Physical Therapist to discuss your concerns and ensure Uncommon Physical Therapy is best for you
(we know it will be)!







